Normal blood pressure for most adults is considered to be between 90/60 and less than 120/80 mm Hg (millimetres of mercury), representing the force your blood exerts against artery walls as your heart beats and rests (American Heart Association). When you look at a blood pressure chart, you’ll notice two distinct numbers — the systolic (upper) and diastolic (lower) values — that together paint a complete picture of how efficiently your cardiovascular system functions.
Your systolic reading measures pressure during heartbeats when the heart muscle contracts forcefully, pushing blood through arteries to nourish tissues and organs throughout your body (MedlinePlus). The diastolic number, on the other hand, captures the pressure between beats when your heart relaxes and refills with blood. Both measurements matter tremendously because elevated readings in either category can signal hypertension, while unusually low values might indicate hypotension (Verywell Health).
How to Measure and Interpret Blood Pressure Readings
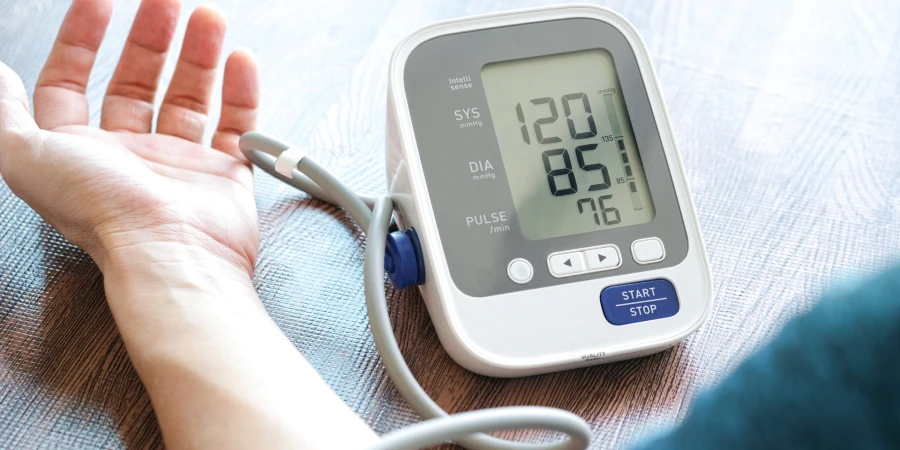
Accurate readings require proper technique and understanding of what the numbers reveal about your cardiovascular health. Always measure blood pressure at the same times each day — typically morning and evening — to establish consistent patterns your healthcare provider can evaluate.
How to check blood pressure
- Before taking a blood pressure measurement, rest quietly for five minutes in a comfortable chair with your feet flat on the floor and your back supported (American Heart Association).
- Place the cuff on bare skin roughly two centimetres above your elbow, positioning your arm at heart level on a flat surface (Blood Pressure UK). Most modern digital monitors automate inflation and deflation, displaying your readings within minutes.
- When measuring, avoid talking, crossing your legs, or moving, as these actions can artificially elevate your readings (Harvard Health).
- Take two or three readings spaced one to two minutes apart, then calculate the average for the most reliable result (Mayo Clinic).
Interpreting the numbers involves understanding where your readings fall within established categories according to the (American Heart Association). Blood pressure ranges for adults are classified as follows:
| Category | Systolic (mm Hg) | Diastolic (mm Hg) |
| Normal blood pressure | Less than 120 | Less than 80 |
| Elevated | 120-129 | Less than 80 |
| High blood pressure Stage 1 | 130-139 | 80-89 |
| Stage 2 Hypertension | 140 or higher | 90 or higher |
| Hypertensive Crisis | Higher than 180 | Higher than 120 |
Elevated readings suggest you’re at increased risk of developing full hypertension unless lifestyle modifications are implemented promptly. Blood pressure levels in the Stage 1 hypertension category typically warrant lifestyle changes and possibly medication, while Stage 2 requires more robust intervention (Harvard Health).
Never ignore consistently raised blood pressure readings, as untreated hypertension can seriously damage your health over time.
A single elevated reading does not automatically mean you have hypertension — multiple measurements taken on different days provide a clearer picture of your typical blood pressure parameters (American Heart Association). Healthcare providers generally diagnose high blood pressure only after documenting elevated readings across several appointments or via home monitoring over weeks.
Blood Pressure Chart by Age
Normal blood pressure varies considerably, particularly during childhood development, though current guidelines recommend the same targets for all adults regardless of age. For adults, the (American Heart Association) established unified targets in 2017, eliminating previous age-based categories. This change resulted from research showing that adults of all ages benefit from maintaining readings below 130/80 mm Hg (Harvard Health). However, average readings do tend to rise with age, especially after 50, as arteries naturally stiffen and plaque accumulates over decades (Verywell Health). The table below shows typical blood pressure values based on age group.
Normal blood pressure by age
| Age Group | Systolic (mm Hg) | Diastolic (mm Hg) |
| Newborns (0–1 month) | 60–90 | 20–60 |
| Infants (1–12 months) | 87–105 | 53–66 |
| Toddlers (1–2 years) | 95–105 | 53–66 |
| Preschoolers (3–5 years) | 95–110 | 56–70 |
| School-aged children (6–12 years) | 97–112 | 57–71 |
| Adolescents (13–17 years) | 112–128 | 66–80 |
| Young adults (18–29 years) | 90–120 | 60–80 |
| Adults (30–39 years) | 90–120 | 60–80 |
| Adults (40–59 years) | 90–120 | 60–80 |
| Older adults (60+ years) | 90–130 | 60–80 |
Normal pressure for someone in their twenties differs from typical readings in older adults, even though treatment targets remain the same. Data from (Baptist Health) shows that men aged 18–39 average 119/70 mm Hg, while women in the same age bracket usually measure 110/68 mm Hg. By age 60 and beyond, these averages are 133/69 mm Hg for men and 139/68 mm Hg for women (Heart Research Institute Australia). These higher averages do not indicate healthy targets but reflect the reality that systolic pressure rises as large arteries lose elasticity with age (Harvard Health).
On average, systolic blood pressure rises steadily with age, but the ideal target remains below 130/80 mm Hg for long-term health.
Symptoms of High Blood Pressure

High blood pressure symptoms rarely show until readings reach dangerously high levels, earning hypertension its reputation as the “silent killer” (Mayo Clinic). Most people with persistently high readings feel perfectly fine, which makes regular screening absolutely vital for early detection and prevention of serious complications.
The absence of noticeable symptoms means many remain unaware that their cardiovascular system operates under harmful strain.
When is blood pressure considered high enough to trigger symptoms?
When blood pressure rises to extreme levels — usually above 180/120 mm Hg — some experience a hypertensive crisis (Healthline). Symptoms during these emergencies may include abrupt severe headaches, difficulty breathing, chest pain radiating to the back, vision disturbances or blurred vision, profound weakness, numbness in limbs, confusion, and nosebleeds (Medical News Today). These signs demand immediate medical attention as they show organs may already be suffering damage (American Heart Association). According to research published by (Healthline), most people do not notice anything unusual until systolic readings exceed 180 mm Hg or diastolic are above 120 mm Hg. Even at these dangerous levels, some remain asymptomatic while their cardiovascular system suffers progressive harm (Medical News Today). This highlights why you cannot rely on how you feel to decide whether your blood pressure needs attention — regular measurement is the only reliable detection method (Mayo Clinic).
High blood pressure often shows no symptoms and may only be found during routine check-ups, so regular checks are essential.
Symptoms of Low Blood Pressure

Low blood pressure chart values below 90/60 mm Hg characterise hypotension, though many healthy, fit people maintain readings in this range without adverse effects (Mayo Clinic). Unlike hypertension, low pressure mostly becomes concerning when it produces noticeable symptoms or indicates an underlying condition (Cleveland Clinic).
Common symptoms include dizziness or lightheadedness, particularly when standing quickly from sitting or lying (orthostatic hypotension) (Vinmec). You might feel blurred or faded vision, fatigue or weakness, difficulty concentrating, nausea, cold or clammy skin, rapid shallow breathing, and increased thirst (Mayo Clinic). According to (Mayo Clinic), a sudden drop of just 20 mm Hg can trigger these uncomfortable sensations, especially if it happens quickly.
If you feel dizzy or faint when standing up, moving slowly and staying hydrated may help reduce symptoms.
Severe hypotension can progress to shock — a life-threatening emergency needing immediate intervention. Signs of shock include profound confusion (especially in older adults), extremely cold and pale skin, rapid weak pulse, and very shallow breathing (Mayo Clinic). When blood pressure drops to critically low levels, organs become deprived of oxygenated blood, which can cause irreversible harm (Cleveland Clinic).
Blood Pressure Levels in Children

Pediatric blood pressure assessment needs a specialised blood pressure chart by age and height percentile, as readings that would worry doctors in adults may represent normal development in younger patients (Baptist Health).
What is normal blood pressure for a child?
Sesame Care offers extensive guidelines factoring in these variables, recognising that cardiovascular maturation follows expected patterns throughout childhood and adolescence.
- Newborns generally show readings around 64/41 mm Hg in their first month, gradually increasing as they grow (Baptist Health).
- By school age (5–10 years), normal systolic values range from 97 to 112 mm Hg, with diastolic readings between 57 and 71 mm Hg (Sesame Care).
- Adolescent blood pressure parameters approach adult levels, with normal ranges of 112–128 mm Hg systolic, and 66–80 mm Hg diastolic (CommonSpirit Health).
Healthcare practitioners use growth charts plotting these factors to decide whether a child’s readings are within the expected range. Parents should ensure their children have regular blood pressure checks starting at age three, as early detection of hypertension in youth allows intervention before cardiovascular damage builds up (Mayo Clinic).
If a child’s blood pressure readings are consistently outside the normal range, speak with a healthcare professional for advice.
Treatment For High Blood Pressure

Managing abnormal blood pressure involves both lifestyle changes and medication tailored to individual circumstances, risk factors, and severity (International Society of Hypertension). Treatment starts with comprehensive lifestyle changes, which form the basis for managing hypertension whether or not medication becomes necessary.
Research published in the (International Society of Hypertension) emphasises that healthy behavioural changes should precede or accompany medication. These changes include:
- Limiting sodium intake to less than 2,300 mg daily (ideally moving towards 1,500 mg), doing at least 150 minutes of moderate aerobic activity weekly
- Maintaining healthy body weight with a target of at least 5% reduction if overweight, drinking alcohol in moderation (no more than one drink daily for women, two for men)
- Managing stress with meditation or breathing exercises, and following heart-friendly eating habits like the DASH (Dietary Approaches to Stop Hypertension) diet (CDC).
Lifestyle changes such as regular exercise and a balanced diet help lower blood pressure naturally.
If lifestyle changes alone do not suffice, or if initial readings indicate Stage 2 hypertension (140/90 mm Hg or higher), medication becomes necessary to protect organs from long-term harm (Harvard Health). According to Hypertension Canada, pharmacotherapy should commence for adults with blood pressure ≥140/90 mm Hg or for those with systolic readings of 130–139 mm Hg who have high cardiovascular disease risk.
Common medication classes include:
- Diuretics (water pills helping kidneys remove excess sodium and fluid)
- ACE inhibitors (angiotensin-converting enzyme inhibitors preventing blood vessel narrowing)
- ARBs (angiotensin II receptor blockers similar to ACE inhibitors)
- Calcium channel blockers (relaxing vessel muscles), beta-blockers (lowering heart rate and contractility) (Health Direct Australia).
Healthcare providers usually start with single medicines, often a thiazide diuretic, adding other agents if targets aren’t reached (Healthline). Many patients eventually need two or three medicines from different classes to adequately control their readings.
Treatment For Low Blood Pressure
Treatment for hypotension depends on whether symptoms hinder daily activities and quality of life. According to Mayo Clinic, symptomless low pressure rarely needs more than monitoring at routine assessments. When problematic symptoms show, management focuses on increasing blood volume and improving circulation (European Society of Cardiology).
Non-medicinal approaches work well for many people and should be tried before considering medication:
- Increasing salt intake can help retain fluid and raise blood pressure, though this should be medically supervised because extra sodium can harm those with certain conditions (Mayo Clinic).
- Drinking more water during the day boosts blood volume, tackling a common cause of hypotension.
- Wearing compression stockings or abdominal binders helps blood return from the legs to the heart, especially benefitting those with orthostatic hypotension (European Society of Cardiology).
Low blood pressure can often be managed with simple lifestyle adjustments like more fluids and gradual movement.
Medication becomes needed if conservative measures do not relieve symptoms sufficiently. Fludrocortisone acetate, a synthetic steroid, helps retain fluid by affecting sodium and potassium balance, increasing blood volume and pressure (Mayo Clinic). Midodrine causes blood vessel constriction, raising readings in those with orthostatic hypotension. For people whose low blood pressure is due to other prescribed medications, adjusting doses or switching drugs often solves the problem (StatPearls).
Possible Complications of Abnormal Blood Pressure

Ongoing abnormal blood pressure — whether high or low — poses serious risks to many organs, with consequences from gradual decline in function to sudden life-threatening events.
Hypertension
Hypertension damages arteries with continuous excessive force on vessel walls, causing thickening, stiffening, and narrowing over years or decades (American Heart Association). This arterial injury sharply increases your risk for coronary heart disease, which develops when heart muscle supply vessels become blocked, potentially triggering heart attacks (Mayo Clinic). Research in (Circulation Research) shows hypertension contributes to heart failure — where the heart is too weak to pump blood efficiently enough for your body’s needs.
“Long-term, untreated hypertension is one of the most significant risk factors for heart attack and stroke.” — British Heart Foundation
Haemorrhagic Stroke
Uncontrolled high blood pressure presents major danger to your brain, acting as a lead cause of both ischaemic (blockage-related) and haemorrhagic (bleeding-related) stroke (American Heart Association). Research in (Circulation Research) indicates the risk of cardiovascular disease rises sharply with higher blood pressure, even at levels once considered acceptable. Beyond sudden incidents, chronic hypertension speeds cognitive decline and substantially boosts dementia risk from cumulative small vessel damage.
Kidney Function Complications
Kidney function deteriorates progressively under persistent high pressure, as delicate filtering structures become scarred and malfunction (Mayo Clinic).
High blood pressure is a top cause of kidney failure needing dialysis or a transplant. Research in (Circulation Research) shows hypertension and chronic kidney disease worsen each other in a vicious circle.
Your eyes feature tiny blood vessels especially vulnerable to pressure damage. Hypertensive retinopathy can cause bleeding, sight loss, and even blindness if ongoing high blood pressure isn’t treated (Mayo Clinic).
Serious hypotension also presents dangers, mainly through insufficient oxygen and nutrient supply to vital organs. When blood pressure suddenly drops or remains chronically low, your brain may not receive enough blood, leading to dizziness, fainting, falls, and in extreme instances, shock requiring emergency intervention (Mayo Clinic).
Persistent abnormal blood pressure can harm the heart, kidneys, brain, and eyes, even without symptoms.
How to Maintain Healthy Blood Pressure

Preventing abnormal blood pressure means proactively adopting healthy habits to keep cardiovascular function and arterial flexibility intact through your lifetime. These strategies work best if started early, before hypertension develops, though they still help at any stage.
Dietary choices
Diet has a major impact on blood pressure. Following eating patterns such as the DASH diet — rich in vegetables, fruits, whole grains, lean proteins, nuts, seeds, and low-fat dairy while reducing saturated fats, refined sugars, and processed foods — has been shown to lower readings significantly (CDC). Sodium reduction is especially crucial, with intake targets below 2,300 mg daily and ideally closer to 1,500 mg for optimal blood pressure control (NHLBI). Reading nutrition labels is important, since most dietary sodium comes from packaged and restaurant foods rather than added salt.
Prepare more home-cooked meals and choose fresh ingredients to better control your sodium intake.
Regular physical activity
Regular exercise strengthens your heart muscle, letting it pump blood efficiently with less effort, thus less force against artery walls (Mayo Clinic). Guidelines recommend at least 150 minutes of moderate-intensity aerobic exercise (like brisk walking) or 75 minutes of vigorous activity weekly (CDC). Even small increases in daily movement — taking stairs instead of lifts, parking further away, adding short walks — meaningfully support cardiovascular health.
Healthy Body Weight
Maintaining healthy weight directly lowers blood pressure, and research finds losing even 5 pounds produces measurable reductions in readings (Mayo Clinic).
Extra weight forces your heart to work harder, increases artery stiffness, and raises inflammation that damages blood vessels (CDC). Achieving and keeping proper weight through balanced diet and regular activity is among the best prevention strategies available.
Weight loss is especially beneficial for adults with raised blood pressure, even with modest reductions.
Stress Management
Stress management is important since chronic psychological pressure triggers hormone responses that acutely raise blood pressure and may contribute to sustained hypertension over time (International Society of Hypertension). Adding relaxation like meditation, deep breathing, yoga, or mindfulness helps moderate your body’s stress response and supports cardiovascular health. Enough sleep — typically seven to nine hours nightly for adults — also plays a protective role (CDC).
Limiting Alcohol Consumption
Limiting alcohol to moderate levels (no more than one drink daily for women, two for men) and avoiding tobacco in all forms protects vessels from injury and inflammation that cause hypertension (International Society of Hypertension). If you smoke, quitting may be the single most impactful action for your overall cardiovascular health (American Heart Association).
“Stopping smoking and cutting back on alcohol are two smart steps towards keeping healthy blood pressure.” — NHS UK
When to Consult a Doctor About Blood Pressure
Knowing when your blood pressure readings or symptoms need professional attention assures prompt intervention before serious complications arise. Scenarios vary from standard monitoring to immediate emergency care:
- Children should have blood pressure checks from age three during regular well-child visits (MedicineNet).
- Set up routine screening starting at age 18, with readings at least every two years if values are always normal and you lack cardiovascular risk factors (Mayo Clinic).
- Once you reach 40, annual screening is sensible, and those with hypertension or heart disease risks should monitor more often as advised by their provider (Mayo Clinic).
Write down your blood pressure readings at home and share them with your GP during appointments.
When is blood pressure considered high enough to contact your doctor?
If home monitoring shows consistent readings of 130/80 mm Hg or higher taken on several occasions over days or weeks, book a professional evaluation (Harvard Health). But don’t panic about one high reading, as brief spikes can occur from stress, exercise, pain, or caffeine consumption (MedlinePlus).
If you have high blood pressure symptoms such as frequent headaches, nosebleeds, vision changes, dizziness, or chest discomfort alongside high readings, contact your healthcare provider quickly rather than waiting for your next routine review (Mayo Clinic).
For hypotension, seek advice if you get frequent dizziness, fainting spells, severe fatigue, blurred vision, or find it hard to concentrate, as these suggest poor blood supply to vital organs (Mayo Clinic).
When Emergency Care Becomes Essential

Quick emergency care is absolutely necessary if readings reach 180/120 mm Hg or higher with worrisome symptoms. According to (American Heart Association), call 999 immediately if your blood pressure exceeds 180/120 mm Hg and you experience chest pain, severe breathlessness, back pain, numbness or weakness (especially on one side), impaired vision, speech difficulty, confusion, or bad headache. These signs point to a hypertensive emergency where organs are in active danger and any delay risks permanent disability or death (Mayo Clinic).
Sudden major drops in pressure with cold clammy skin, rapid breathing, weak pulse, or confusion are true emergencies and may indicate shock (Cleveland Clinic).
Call emergency services immediately if severe symptoms appear with very high or very low blood pressure.
How This Article Was Researched
This guide was developed by the Suplint research team using up-to-date data from peer-reviewed journals and reputable health institutions. The team analysed medical studies and recommendations on cardiovascular health to ensure that all insights are science-based, practical, and up to date. Every source cited in this article comes from leading authorities in the field, reflecting current findings published in the last five years. Please remember: this content does not replace professional medical advice. For questions regarding your health, dietary habits, or supplement choices, always consult your healthcare provider.
References
- American Heart Association: https://www.heart.org/en/health-topics/high-blood-pressure/understanding-blood-pressure-readings
- Mayo Clinic: https://www.mayoclinic.org/diseases-conditions/high-blood-pressure/in-depth/high-blood-pressure/art-20047889
- CDC: https://www.cdc.gov/high-blood-pressure/prevention/index.html
- Harvard Health: https://www.health.harvard.edu/heart-health/reading-the-new-blood-pressure-guidelines
- MedlinePlus: https://medlineplus.gov/lab-tests/measuring-blood-pressure/
- Blood Pressure UK: https://www.bloodpressureuk.org/your-blood-pressure/how-to-lower-your-blood-pressure/monitoring-your-blood-pressure-at-home/how-to-measure-your-blood-pressure-at-home/
- International Society of Hypertension: https://pmc.ncbi.nlm.nih.gov/articles/PMC10713007/
- Medical News Today: https://www.medicalnewstoday.com/articles/270644
- Heart Research Institute Australia: https://www.hri.org.au/health/learn/risk-factors/what-is-normal-blood-pressure-by-age
- Cleveland Clinic: https://my.clevelandclinic.org/health/diseases/21156-low-blood-pressure-hypotension
- Circulation Research: https://www.ahajournals.org/doi/10.1161/CIRCRESAHA.122.321762
- Hypertension Canada: https://hypertension.ca/wp-content/uploads/2025/05/Hypertension-guideline.pdf






